by Stephanie Lopes
The Ito Family decided to do something and saved their 20-month-old daughter’s life, as told by Mike and Daeni Ito of Maui.
Mike: It was just after midnight on the night of our 7th wedding anniversary when Cobie, our then 20-month-old daughter, made an innocent coughing sound. Thousands of coughs like this I normally overlook, but something made me decide to check the baby monitor.
I saw that her eyes were open, but her arms were moving in an unusual, repetitive, up-and-down motion. After a few seconds, I noticed these movements getting progressively smaller. I went to peek in her room, and when she didn’t react to me coming in, I immediately turned on the light.
What I saw was something now forever burned into my memory. Cobie’s movement had stopped; her face was blue, and her eyes were rolling towards the back of her head. I grabbed her limp body from the crib, and I screamed for my wife Daeni who was sleeping. As I yelled for her, I tried to do something but had no idea what was wrong and wasn’t thinking clearly.
Daeni: I was abruptly awoken out of sleep, and I didn’t really know what was going on. As soon as I took Cobie from my husband, he immediately dialed 911. I thought she would just snap out of it. I thought she had choked because she was blue and not responsive.
Since I took my CPR refresher course at Kahului Fire Station just the day before, CPR was so fresh in my mind. I had firefighters Scott Pires, Matt Pires and Ken Tsuhako talking to me in my head: “Just do something. Someone who doesn’t want CPR will not let you do it.” As a nurse, you think about oxygen to the brain and vital organs and every second counts; it wasn’t more than 15 seconds until I got her to the ground and started doing chest compressions.
Mike: Cobie’s color returned after a couple of minutes of doing chest compressions, but she was still unresponsive, and her eyes continued to roll around blankly.

After what seemed like forever, but was really just a few minutes, two police officers and the paramedics arrived. Daeni and Cobie were loaded into the ambulance. Somewhere between Kula and the hospital, Cobie finally gave out a good cry and started to regain awareness – about 20 minutes after we initially found her. In the meantime, our 4-year-old daughter, Kenna, miraculously slept through it all.
After spending the rest of that day and the next in the hospital, Cobie was sent home. Since then, we’ve had follow-ups with a couple of specialists and our great pediatrician, Dr. Steve Clark. Cobie’s doctors think she probably suffered from a febrile seizure, which could have caused her to go into cardiac arrest and stop breathing. Everything has checked out fine, though there still is no certainty on the cause or likelihood of recurrence, nor do we know what would have happened had we not checked on her and performed immediate chest compressions.
Daeni: Cobie is now active and rambunctious with her own personality and purpose. She fills our lives with joy and happiness.
Many would say we were very unlucky for our situation; I say we are so lucky to have our Cobie still here with us today. We are grateful for her. We are also grateful for the Kahului Airport Firefighters, Dr. Steve Clark, and Pamela Foster of the AED Institute, who steered us in the right direction for specialty care and helped me become an American Heart CPR instructor.
We realize our story could have turned out very differently, so we would like families to be prepared in order to strive for positive outcomes!

Sudden Cardiac Arrest
According to Pamela Foster, a registered nurse and President of the AED Institute and Executive Director of the non-profit Kids4CPR, “These stories occur on our island every day, maybe five to six times per day. The victims can be any age, appear to be in good health, and doing everyday activities.”
Sudden cardiac arrest is an electrical problem in the heart that causes it to beat irregularly – or fibrillate – and stop pumping blood. A victim suddenly passes out and is not awake nor breathing normally; their eyes can be open, they might be making jerking actions, or they may not be moving, moaning, or groaning.
Sudden cardiac arrest can happen to anyone of any age at any time. In fact, there are several inherited, genetic conditions that can cause sudden cardiac arrest in children. These heart diseases in children are sometimes characterized by these common symptoms:
- Fainting or sudden collapsing.
- Feeling of rapid heart rate when not appropriate/at rest.
- Dizziness or chest pain, especially during exercise.
- Fatigue or tiring easier than others.
The AED Institute believes there are as many as 1,600 children in Hawaii that have an inherited heart condition that could cause a heart rhythm problem and result in sudden cardiac arrest. However, sudden cardiac arrest can be prevented in most children if the condition is known and if an appropriate medical specialist sees the child.
Do Something
“Cardiac arrest survival rates in Hawaii are much like the rest of the country – about 5 to 6 percent. But it does not need to be that way, as we have a 70 percent survival rate within our Hawaii Airports, thanks to easily accessible AEDs and free CPR classes,” says Foster.
There are two priorities that are proven to save lives: immediate high-quality chest compressions and immediate use of an AED.
According to the American Heart Association, “If no bystander CPR is provided, a victim’s chances of survival are reduced by 7-10 percent with every minute of delay.”
Bystander CPR is simple. First, check if the person is breathing or responsive. If they are not responsive, call 911 and then push hard and fast in the center of the chest and only stop if the person says “ouch” or if EMS says, “We will take over.”
“It is better to do chest compressions on someone who may not need them, then to not do the compressions on someone who does need them,” says Foster.
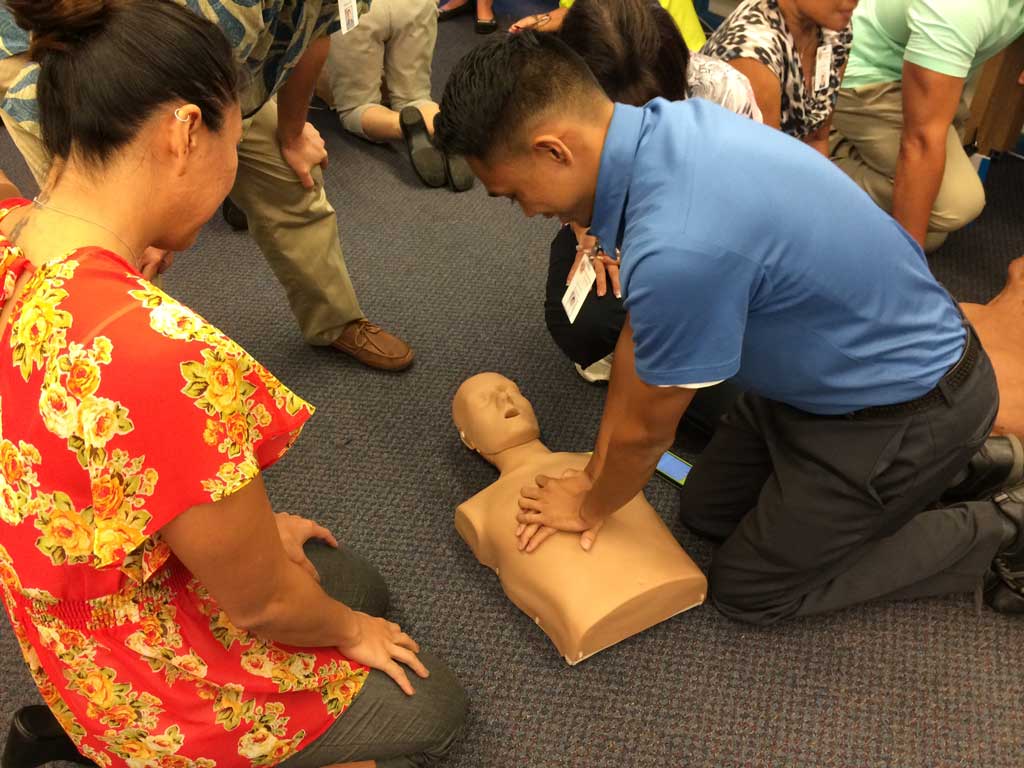
For adult CPR, the base of the hand goes on the middle of the chest with the other hand on top. Shoulders should be directly over your hands, and elbows should be locked; use your whole body to do strong compressions at a pace of 100 to 120 times a minute.
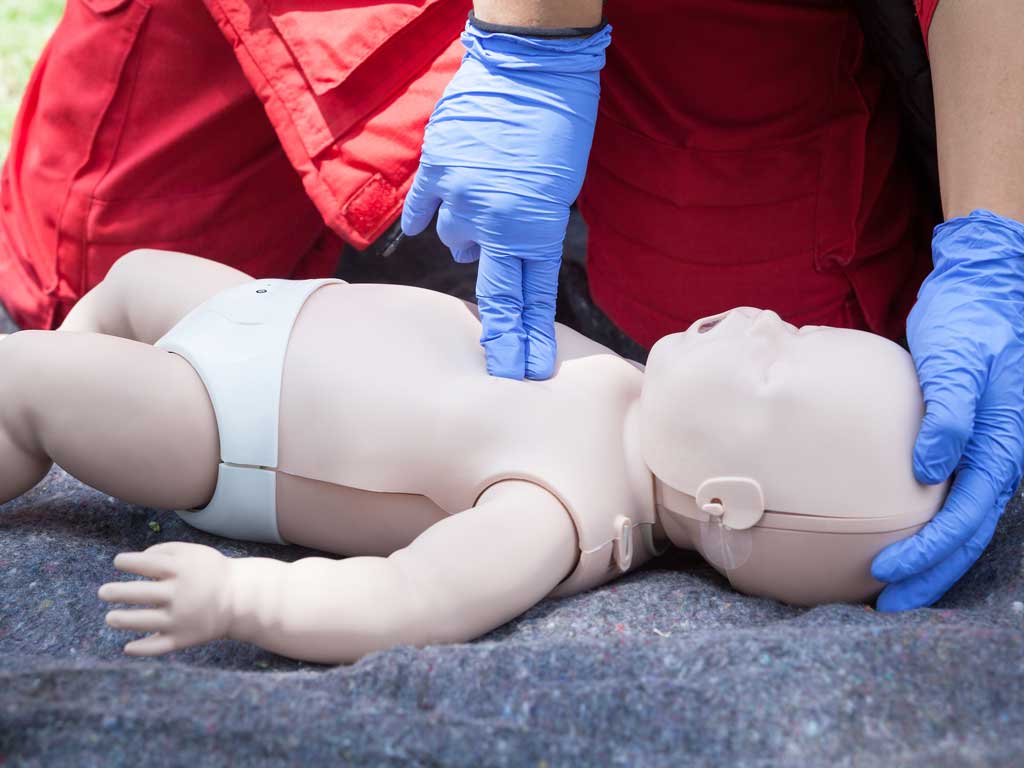
For smaller children, you can use one hand and for very young infants (four weeks to one-year-old) two fingers. Strong compressions are important – about one-third to one-half the depth of the chest, which is two inches deep for an adult and 1.5 inches deep for a child. “It is better to push too hard, than not hard enough,” says Foster.
Two light breaths – “only a puff of air” – can be administered to small children after thirty compressions, but “make sure you are on the chest pushing as much as possible,” says Foster.
“Chest compressions help buy the victim time until the AED arrives. By pushing hard and fast in the center of the chest, the rescuer is helping to circulate the blood and oxygen to the brain and heart,” Foster emphasizes. “If you stop the compressions for any reason, the blood stops circulating.”
The American Heart Association has promoted hands-only CPR since 2008, Foster clarifies, “It is not really the breaths that make or break the survival rate; it is the long pauses that occur when bystanders are trying to get those breaths in. The victim is usually full of oxygen when they collapse – about four to six minutes worth – so they need chest compressions, not breaths, and for every couple of seconds you are off the chest, you are not pushing the blood to the brain, leading to less chance of survival.”
Automated External Defibrillators (AEDs), which can be found in all Hawaiian airports, McDonalds, and many other public places, can be used in addition to chest compressions if obtained. An AED is a device utilized to administer an electric shock through the chest wall to the heart. Built-in computers assess the patient’s heart rhythm, judge whether a shock is needed, and then administer it if necessary. An AED will not deliver a shock if not necessary, and with its included simple audio and visual instructions, it is apparent AEDs are designed to be used by non-medical personnel. An app called PulsePoint AED can be downloaded on devices to show the nearest AED to your current location.
The steps to save a life during a cardiac arrest are simple:
- C = Call 911 and send someone for an AED.
- P = Push hard and fast in the center of the chest at about 110 times per minute, which corresponds to the beat of the classic disco song “Stayin’ Alive.”
- R = Repeat chest compressions and then respond with an AED until EMS arrives. If you can call 911 and start high-quality chest compressions, you may double, triple, or perhaps even quadruple the victim’s chance of survival.
- The success of calling 911, grabbing an AED and immediately administering compressions is confirmed in our Hawaii community. Foster sites numerous examples from her work, which includes teaching CPR to 5th graders in more than 150 local schools at no charge: “There have been over 60 survivors in the Hawaii airport system, and now there are mandatory AEDs in the City and County offices with more than a half a dozen survivors in the last couple of years.”
Learn More
“My advice to parents would be take a CPR/First Aid class ASAP!” exclaims Daeni. “I needed CPR for my career as an RN, but ended up using it for my life as a mom.”
The AED Institute offers frequent classes; simply view the class calendar at www.aedinstitute.com
Foster adds, “You do not need to be certified to save a life; you only need to have the knowledge and confidence to act.” The knowledge of calling 911 and pushing hard and fast in the center of the chest seems simple, so, if witnessing a cardiac arrest, do something!
Concerns and Questions
Common CPR Fears—Nullified
If hesitations still exist about doing something when witnessing someone who is non-responsive, realize there is no reason not to call 911 and start compressions.
What if they get better?
I should just wait and see. “Call 911,” stresses Daeni, “If you don’t need it, it’s ok, but what if you really needed it? You want to always think you did everything to help.” For every second that passes without action, a person’s chance of surviving a cardiac arrest lessens.
I don’t want to hurt the person.
About 75 to 80 percent of all sudden cardiac arrests happen at home, so some may be fearful of hurting their grandparents, young child, or even pregnant wife. “The victim is dead. If you do nothing, you certainly cannot do worse than that,” states Foster. Hard and fast chest compressions are necessary to circulate blood and oxygen to the heart. If the person does not need CPR, they will say “ouch” and will likely not be angry at a rescue attempt.
What if I do something wrong?
The Hawaii Good Samaritan Act protects against liability, and you do not need to be certified to administer chest compressions. “You cannot do anything wrong,” Foster adds. “Our survival rates can only go up.”
I don’t want to catch a disease.
Since there are no breaths involved in hands-only CPR, the likelihood of catching a disease is minimal.





